Beyond Healthcare
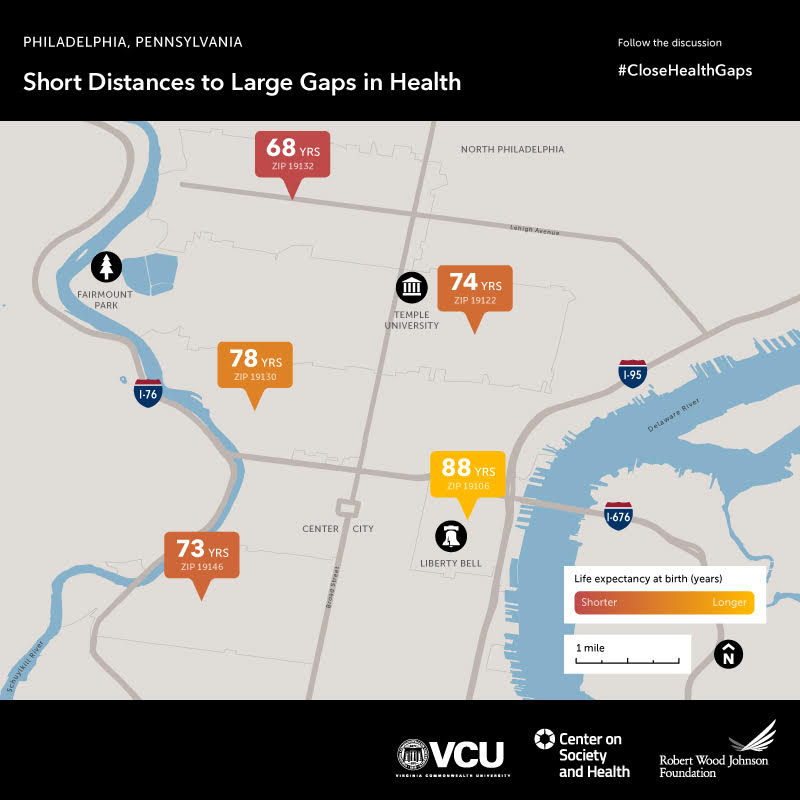
expectancy in different zip codes
In college, I studied medical anthropology, a discipline that examines health and illness from social, cultural, and historical perspectives. My experiences as a patient advocate with the National Health Corps Philadelphia has expanded on and enriched what I’ve learned in the classroom. It’s viscerally shown me the urgency of predicaments affecting disenfranchised people, and encourages me to continue exploring what community-based health advocacy really means.
The other PDPH advocates and I usually meet patients when they’re at the end of their line-- helping them get medications that a broken insurance system failed to, often in order to treat illnesses that could have long been prevented. Through our service year, we have had to face a hard truth: in an ideal world, our positions at the health centers would not exist. An ideal world would not have vulnerable lives rely on a cobbled-together network of programs whose benefits and eligibility requirements remain at the whim of pharmaceutical corporations. What does an ideal world look like then? And what is my and our place in helping to make that world a reality?
Serving in Philadelphia, I’ve been reflecting more on the various ways broader social injustices shape local places and cultures. As a patient advocate, I split my time between Strawberry Mansion Health Center, which serves predominantly African-American patients in the surrounding neighborhood, and Health Center 10, located in a diverse immigrant community in Northeast Philadelphia. The history of medical racism and violence against African-Americans presents unique challenges for staff and patients at Strawberry Mansion. The language barriers and citizenship status of many patients at Health Center 10 render insurance and other benefits more inaccessible to them.

The neighborhoods of both clinics lack adequate walkable green spaces for exercise and outlets for healthy food, contributing to high rates of chronic illness. Residents additionally face impoverishment from gentrification and discriminatory development. While these issues manifest distinctly in each neighborhood, I’ve witnessed parallel trends in parts of the California Bay Area, where I went to college, and in Austin, Texas, where I grew up.
When a patient has reached the doctor’s office, oftentimes it is already too late. The illnesses treated by health professionals are frequently symptoms of larger social inequities. We can see these inequities on the streets, in the ways cities are planned, in policies and systems that implicitly or explicitly value some lives over others, and in the ever-present force of history undergirding discrimination and bias in virtually all aspects of society.
I believe there is so much latent potential for medical professionals to leverage their social, intellectual, and material privilege beyond conventional healthcare contexts. I’m inspired by fellow NHC members who serve in integrated medical settings that aim to mitigate food insecurity or housing precarity; who meet people where they are-- on streets, in schools, in community centers-- before it’s too late. I’m especially excited by what health professionals can achieve when they engage with policy and urban planning initiatives. We have yet to realize how far we can go to ensure that everyone, especially the most marginalized, has the opportunity to offer their best selves to the world.
